The Risk of Dying From COVID-19
Tuesday May 19, 2020



One of the biggest problems facing the world right now is managing compliance with stay-at-home orders. In brief, we know there are people who are opening businesses, terrorizing government officials, and just saying stupid things. All of these are actively killing people. But they don’t understand it. To help, we need to get our head around the fatality rate.
Let’s start by talking about what people think the fatality rate is. Nonsense like this claiming:
he overall mortality rate decreased to around 0.66%
has been repeated ad nauseum. I’ve taken this quote out of context, but that’s okay. This is the only part anyone paid attention to. Many more are saying it is no worse than the flu, and that’s dumb on two fronts; most of them having never seen the flu, before. Either way, it is hard to explain to people that a 99.34 percent chance of survival just isn’t very good…and that grossly overestimates the survival rate.
The problem is, we are underestimating the expected death toll, by
estimating the fatality rate as a percentage of the total cases.
For instance, using the data from yesterday, May 18, 2020, for the
United States, provided by
Worldometer this gets
us
The naïve approach here is to simply exclude the unknowns from the
calculation. That gets us deathrate
for these countries. This gives us this histogram:
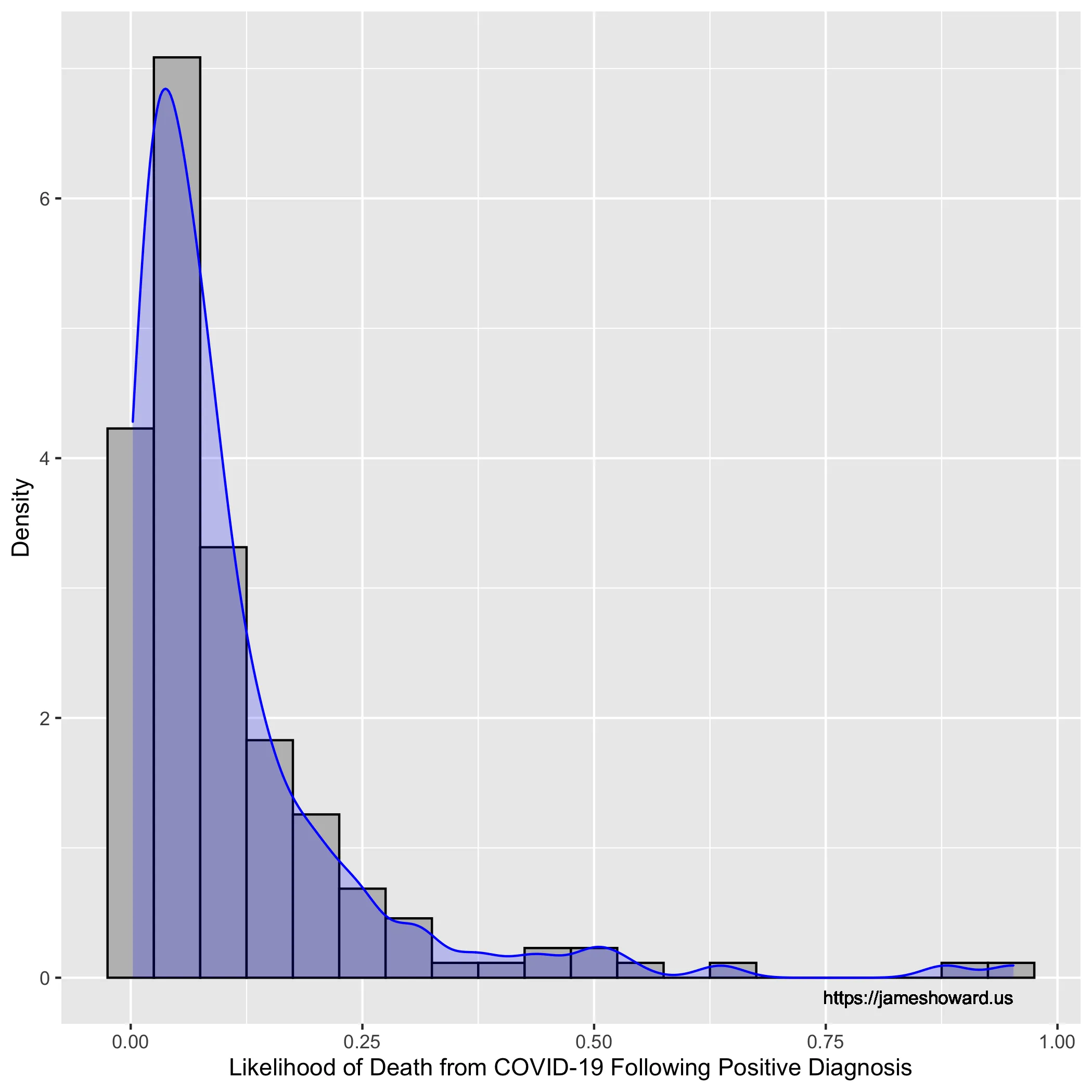
Working with that, we can see there’s quite a long tail on this
distribution. We can, somewhat naïvely still, find the mean of the
deathrate, and that is 10.96 percent.
I think the best way to approach this is to find a weighted mean
where the weights are the percentage of resolved cases for
each country. Mathematically, this is
Applying this metric, we get approximately 7.94 percent fatality rate (95% CI +/- 0.007 percent). That number makes a lot more sense than some of the other estimates out there. From November, 2002, to July, 2003, there were 8096 cases of SARS, globally, resulting in 774 deaths. This is a fatality rate of 9.6 percent. Since 2012, there have been 2519 cases of MERS resulting in 866 deaths, with a net fatality rate of 34.4 percent. Both SARS and MERS are closely related to the virus causing COVID-19, SARS-CoV-2, so these are natural comparison points. On the other hand, COVID-19 is substantially more widespread, with nearly 5 million cases, globally. For another comparison point, CDC’s estimate for influenza during the 2017-2018 season, the worst in the last 10 years, is 44802629 symptomatic cases leading to 61099 deaths. There were probably several million more asymptomatic cases, but setting those aside, the fatality rate for influenza is, at worst, about 0.1 percent. Most years are significantly lower.
Back to COVID-19, of the 1101930 outstanding cases, that results in an additional 87480 (95% CI +/- 70) deaths, and that is before taking into account any additional cases. Given that there is no known treatment for COVID-19, aside from ventilation, as of today, those 87480 deaths are essentially inevitable. The infection is still spreading and that will result in more cases and more fatalities, overall.
This is why it is important to follow the recommendations for social distancing. In short, stay home unless you have to go out. If you have to go out, wear a mask. These two factors, combined, will significantly slow the spread. The likelihood of getting COVID-19 is higher than your likelihood of getting influenza and your likelihood of dying from COVID-19 is substantially higher than you realize if you get COVID-19. The raw case counts, right now, are artificially deflated, globally, because of social distancing measures. Those numbers, lower than the apocalyptic sounding millions of deaths, are evidence social distancing is working, not that it is unnecessary. The smart people right now are upset the numbers are as high as they are, because not enough people held back.
Finally, as a back of the envelope, this has a lot of flaws. The most important of these flaws is applying the global rates to the United States. To put it bluntly, the United States is now a developing nation. We are well below the developed world’s levels of access to health care, education, clean water, and other preventative measures, all of which are important in this crisis. This means that 7.94 percent is a lowball estimate for the United States. While it represents the world figures, the United States, given its resources, cannot be expected to perform at that level. Accordingly, one must expect a higher death rate in the United States, overall.